ACLS Bradycardia Algorithm
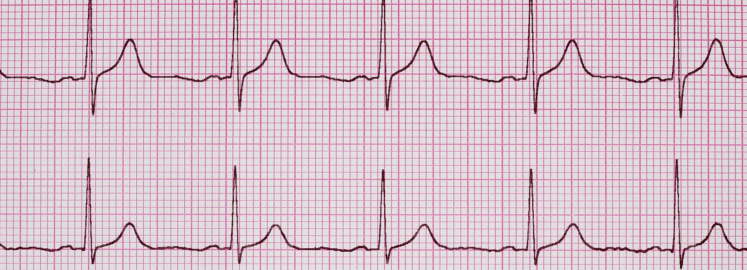
The ACLS bradycardia algorithm is a part of the Advance Cardiac Life Support (ACLS) algorithm used in emergency medicine to manage patients with bradycardia. Bradycardia is a slow heartbeat condition, typically less than 50 beats per minute.
The AHA Bradycardia Algorithm is a structured plan used in Advanced Cardiovascular Life Support (ACLS)
It involves checking the patient for symptoms and figuring out what might be causing the slow heart rate, making sure their airway is clear, keeping an eye on vital signs such as heart rhythm, monitor blood pressure, and oxygen levels, setting up IV access, and giving appropriate treatments like atropine, transcutaneous pacing, or dopamine/epinephrine if needed.
Here's a step-by-step approach of how healthcare providers manage bradycardia using the ACLS (Advanced Cardiovascular Life Support) protocol:
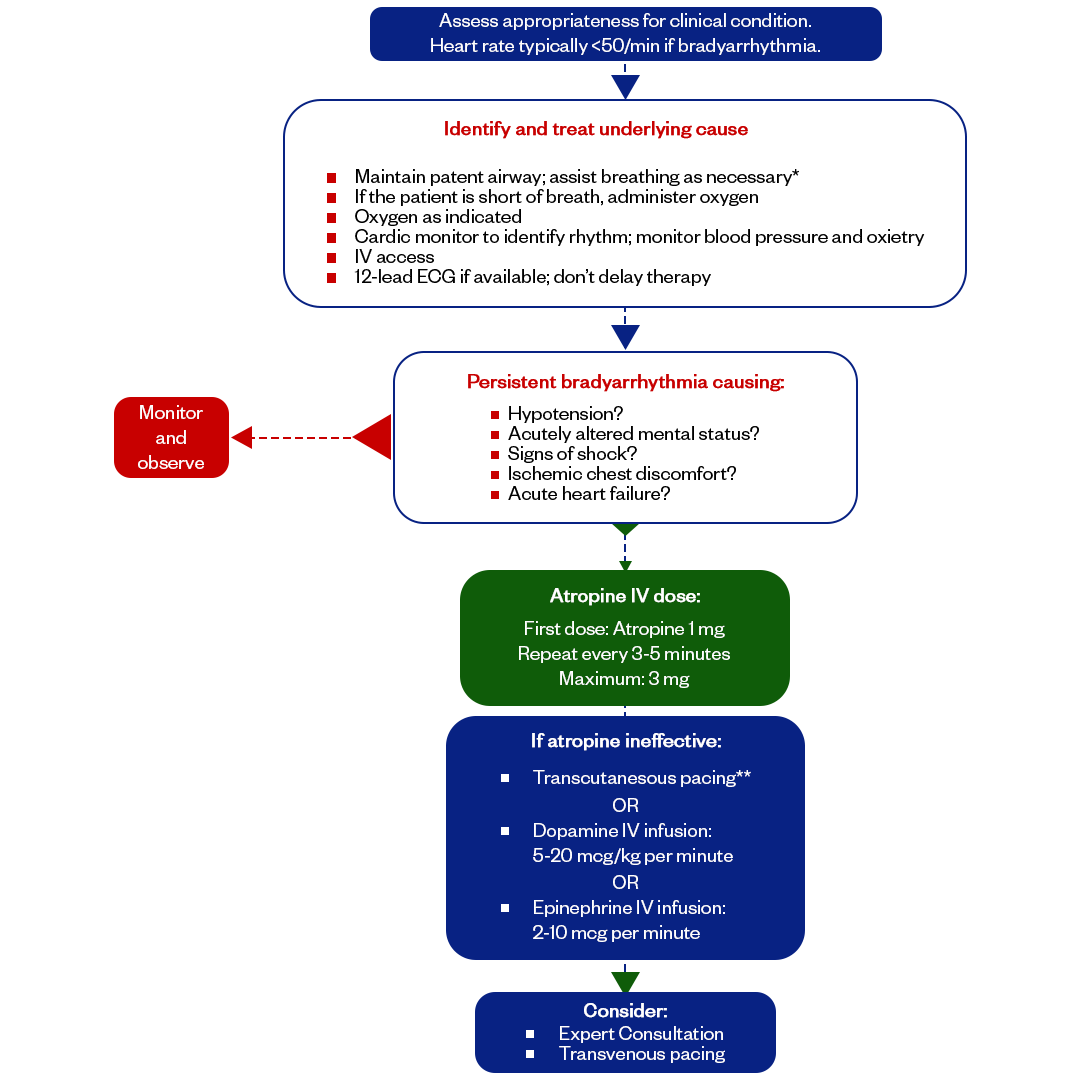
Treatment For The Bradycardia (Algorithmic Approach)
The treatment of bradycardia depends on the clinical condition, symptoms, and the underlying cause of the slow heartbeat of a patient. The treatment is based on controlling the symptoms and identifying the cause using the Hs and Ts of the bradycardia Advanced Cardiac Life Support algorithmic approach. We will later learn about the Hs and Ts, but first, let's look at the surface of bradycardia's treatment.
-
Primary Assessment: Assess the patient's airway, breathing, and circulation (ABCs) and provide appropriate interventions.
-
Monitoring Vital Signs: Monitor the patient's vital signs, including heart rate, blood pressure, and oxygen saturation.
- Identify the Cause:
- Determine the underlying cause of bradycardia, including hypoxia, hypovolemia, acidosis, toxins, cardiac issues (e.g., heart blocks), or other factors.
- Symptomatic vs. Asymptomatic Bradycardia:
- Assess the patient's symptoms. Bradycardia with hemodynamic instability or symptoms like chest pain, altered mental status, hypotension, or signs of shock requires more immediate intervention than asymptomatic bradycardia.
- Atropine:
- If the patient has symptomatic bradycardia with poor perfusion, consider atropine or transcutaneous pacing.
- The typical initial dose for adults is 0.5 mg IV, which can be repeated every 3-5 minutes, up to 3 mg.
- Atropine is primarily used for bradycardia resulting from vagal stimulation or certain medication overdoses.
- Dopamine or Epinephrine:
- Epinephrine and dopamine are second-line drugs for symptomatic bradycardia. If atropine is ineffective or not indicated, consider using a medication like dopamine or epinephrine to increase heart rate and improve cardiac output.
- Dopamine can be infused at 2-20 micrograms/kg/minute.
- Epinephrine can be administered at 2-10 micrograms/minute doses.
- Temporary Cardiac Pacing:
- In cases of severe bradycardia, unresponsive to medications, or if the patient remains unstable, temporary transcutaneous pacing may be necessary.
- Consult a Cardiologist or Specialist:
- If the bradycardia is related to underlying cardiac conduction disorders (e.g., complete heart blocks), consult a cardiologist or electrophysiologist for further evaluation and potential permanent pacemaker placement.
Hs and Ts of Bradycardia ACLS Algorithm
- Hypovolemia
- Hypoxia
- Hydrogen Ion Excess (Acidosis)
- Hypothermia
- Toxins
- Tamponade
- Tension Pneumothorax
- Thrombosis (Pulmonary Embolism)
- Thrombosis (myocardial infarction)
- Trauma
Fast and Convenient
Take ACLS Classes
*Nationally Accepted
ACLS
CERTIFICATION
AHA ACLS course
State-of-the-Art Facilities
Unlimited Exam Retakes
$260
ACLS
ONLINE CERTIFICATION
AHA ACLS Online Course
100% online training
Unlimited Exam Retakes
$280
Bradycardia Algorithm FAQs
What is the Bradycardia Algorithm?
Bradycardia is a situation where your heart beats slower than the normal rate <50 beats per minute, with the presence of symptoms. The AHA Bradycardia algorithm identifies the symptoms and causes to deliver treatment efficiently. The algorithm helps quickly identify the symptoms and underlying causes of bradycardia to ensure timely and effective treatment. It provides a structured approach to determine whether emergency interventions like medications, pacing, or other supportive measures are needed.
What is the most common cause of bradycardia ACLS?
The most common cause of bradycardia in ACLS scenarios is often related to underlying cardiac conduction abnormalities. Abnormalities such as atrioventricular (AV) blocks, Hypothyroidism, Sinus Bradycardia, and medication can lead to slow slow heart rhythm. Bradycardia also causes hypotension (low blood pressure) when enough blood is not circulated effectively.
What is the first intervention for bradycardia?
The initial intervention for bradycardia involves ensuring airway and breathing support, continuous patient monitoring, oxygen supply, blood pressure and oxygen saturation assessment, and establishing intravenous (IV) access. Additionally, obtaining an ECG is crucial for better rhythm visualization and monitoring.
How do you stabilize bradycardia?
Bradycardia is stabilized by first supporting airway and breathing, providing oxygen, monitoring vitals, and getting an ECG. If the patient shows serious symptoms, medications like Atropine, Dopamine, or Epinephrine are used. In some cases, temporary heart pacing may be needed.
What are the symptoms of bradycardia?
Symptoms of bradycardia are:
- Fatigue
- Dizziness
- Fainting
- Shortness of breath
- Chest pain
- Cognitive impairment
- Palpitations
- Weakness
How is Bradycardia Treated in ACLS?
The go-to medication for managing symptomatic bradycardia, according to the ACLS bradycardia algorithm guidelines, is atropine. Doctors typically administer it at a dose of 1 mg through an IV push, and this can be repeated every 3-5 minutes if needed, up to a maximum total of 3 mg. If atropine doesn't work effectively in treating the symptomatic bradycardia, healthcare providers might consider using dopamine as the next option.
Is CPR Given for Bradycardia?
During bradycardia, chest compressions improve blood flow to vital organs, especially the heart and brain. In adults and children receiving CPR, chest compressions are only given when there's no pulse or when organ perfusion is inadequate.

Owner Jeff Haughy has been providing high-quality care in the EMS industry since 1995 and started his Fire Service career with the Alameda Fire Department in 1991 as a Fire Explorer.