Immediate Post-Cardiac Arrest Care Algorithm
In the critical moments following cardiac arrest, delivering immediate and effective care is paramount to patient survival and neurologically intact outcomes. The Immediate Post-Cardiac Arrest Care Algorithm serves as a structured and evidence-based guide for healthcare providers, delineating the crucial steps and interventions required to optimize the chances of successful resuscitation and post-arrest management.
The ACLS algorithmic approach integrates the latest advancements in resuscitation science, emphasizing a seamless transition from cardiopulmonary resuscitation (CPR) to targeted post-arrest care. Ultimately, the algorithm targets enhancing the overall quality of patient care and fostering improved outcomes in the aftermath of cardiac events.
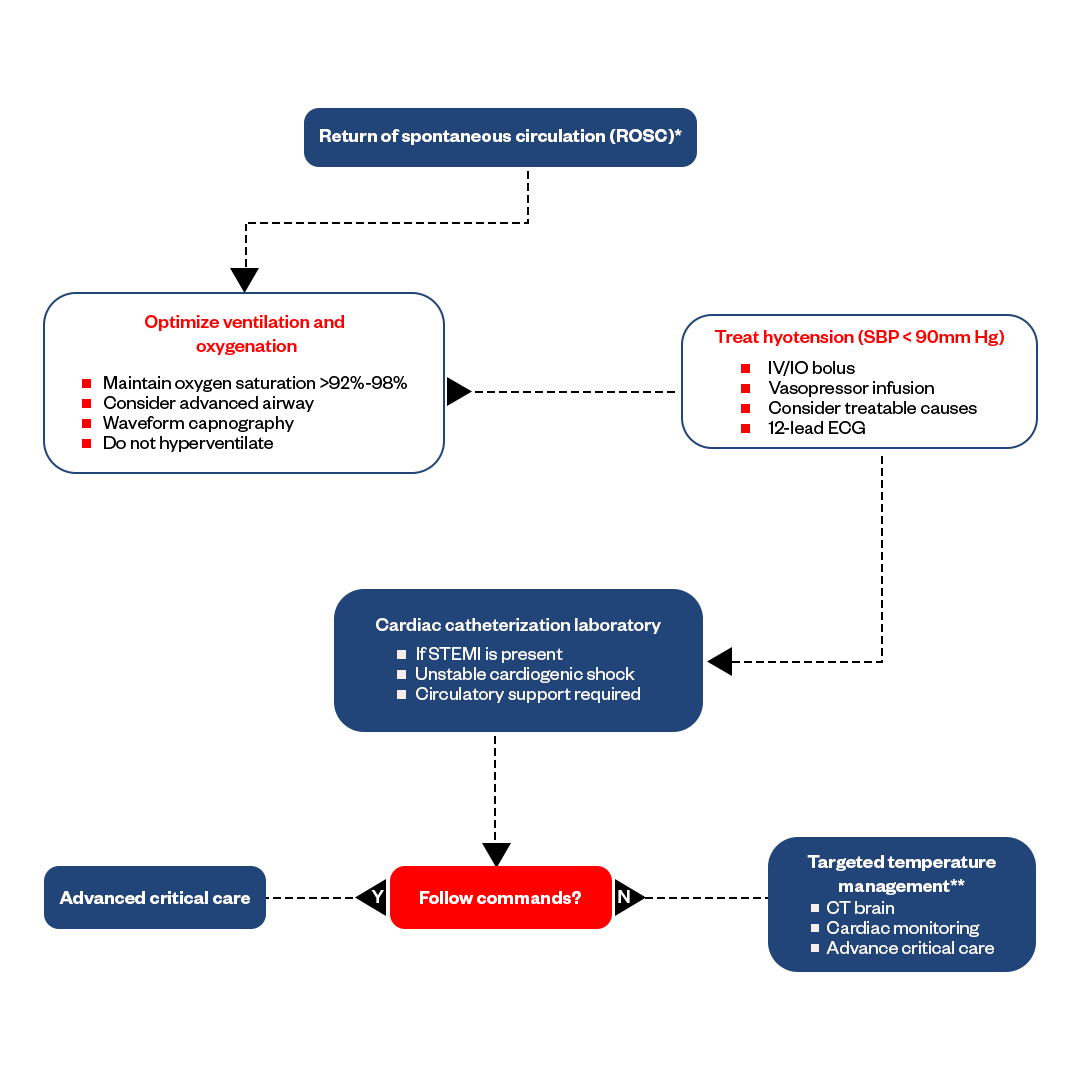
Immediate Post-Cardiac Arrest Algorithm Entails:
Immediate post-cardiac arrest care focuses on the key components often referred to as the "4 Ts," which include Temperature Management, Targeted Temperature Management, Treatment of the Underlying Cause, and Triage.
Temperature Management:
Purpose: Immediate post-cardiac arrest care involves temperature management to mitigate the risk of neurological damage. The rationale behind inducing mild hypothermia is to reduce the brain's metabolic rate, decrease oxygen consumption, and minimize inflammation, thereby protecting against ischemic injury.
Procedure: Targeted Temperature Management (TTM) involves maintaining the patient's body temperature within a specific range, typically around 32-36 degrees Celsius. This can be achieved through various methods, including surface cooling (cooling blankets or pads), intravascular cooling devices, or ice packs. The cooling period typically lasts for 24 hours.
Monitoring: Continuous temperature monitoring is crucial during this phase to ensure the patient stays within the desired temperature range. Invasive temperature monitoring, such as bladder or esophageal probes, is often used for precise control.
Targeted Temperature Management (TTM):
ACLS Targeted Temperature Management (TTM) is a therapeutic strategy employed in post-cardiac arrest care to mitigate neurological injury and enhance patient outcomes. During a designated timeframe, controlling body temperature within a specific range, typically between 32°C and 36°C, helps modulate the inflammatory response and reduce secondary brain injury. TTM is integral to preventing neuronal damage and optimizing neurological recovery after resuscitation, underscoring its pivotal role in the comprehensive approach to post-cardiac arrest care.
Indications: TTM is indicated for comatose survivors of cardiac arrest with return of spontaneous circulation (ROSC) to improve neurological outcomes. It is particularly beneficial in cases of ventricular fibrillation or pulseless ventricular tachycardia.
Duration: The duration of TTM is typically 24 hours, followed by a controlled rewarming phase. This gradual rewarming helps prevent complications associated with rapid temperature changes.
Benefits: TTM has been shown to reduce the risk of neurologic injury and improve survival rates. It helps minimize the reperfusion injury that can occur when blood flow is restored to the brain after a period of ischemia.
Treatment of the Underlying Cause:
Identification: Identifying and addressing the underlying cause of the cardiac arrest is crucial for long-term management. Common causes include acute coronary syndromes, arrhythmias, electrolyte imbalances, and respiratory failure.
Interventions: Prompt interventions may include percutaneous coronary intervention (PCI) for coronary artery blockages, antiarrhythmic medications, and correction of electrolyte abnormalities. Effective treatment of the underlying cause improves the chances of sustained recovery and prevents recurrent cardiac events.
Triage:
Destination Decision: Post-cardiac arrest patients may be transferred to specialized facilities equipped to provide advanced cardiovascular care and neuroprotection. Decisions regarding the appropriate level of care and destination are based on the patient's overall clinical condition, the availability of specialized services, and local protocols.
Neurological Assessment: Neurological assessment is a crucial aspect of triage. This includes monitoring for signs of neurological recovery or complications. Some patients may require ongoing neurocritical care or rehabilitation services.
Step-By-Step Process of Post-Cardiac Arrest Algorithm
Below is a general step-by-step process based on the AHA guidelines for immediate post-cardiac arrest algorithm:
- Confirm return of spontaneous circulation (ROSC).
- Ensure adequate oxygenation and ventilation.
- Monitor vital signs, including blood pressure, heart rate, and oxygen saturation.
- Maintain an open airway and support ventilation.
- Administer 100% oxygen.
- Obtain IV or intraosseous access.
- Consider targeted temperature management (cooling) for eligible patients.
- Perform a systematic assessment to identify and treat the underlying cause of cardiac arrest (e.g., myocardial infarction, hypovolemia, electrolyte imbalances).
- Titrate inspired oxygen to achieve adequate oxygen saturation.
- Optimize ventilation to maintain normocapnia.
- Administer fluids cautiously to optimize intravascular volume.
- Consider vasopressors to achieve and maintain target blood pressure.
- Consider advanced hemodynamic monitoring in selected cases to guide therapy.\
- Assess neurological status regularly.
- Consider neuroimaging and other diagnostic studies if indicated.
- Manage complications associated with post-cardiac arrest syndrome, such as myocardial dysfunction, systemic inflammatory response, and persistent organ failure.
- Consider coronary angiography and percutaneous coronary intervention (PCI) for patients with suspected or confirmed acute coronary syndromes.
- Consider neurological prognostication using multiple modalities.
- Involve neurology or neurocritical care specialists as needed.
Fast and Convenient
Take ACLS Classes
*Nationally Accepted
ACLS
CERTIFICATION
AHA ACLS course
State-of-the-Art Facilities
Unlimited Exam Retakes
$260
ACLS
ONLINE CERTIFICATION
AHA ACLS Online Course
100% online training
Unlimited Exam Retakes
$280