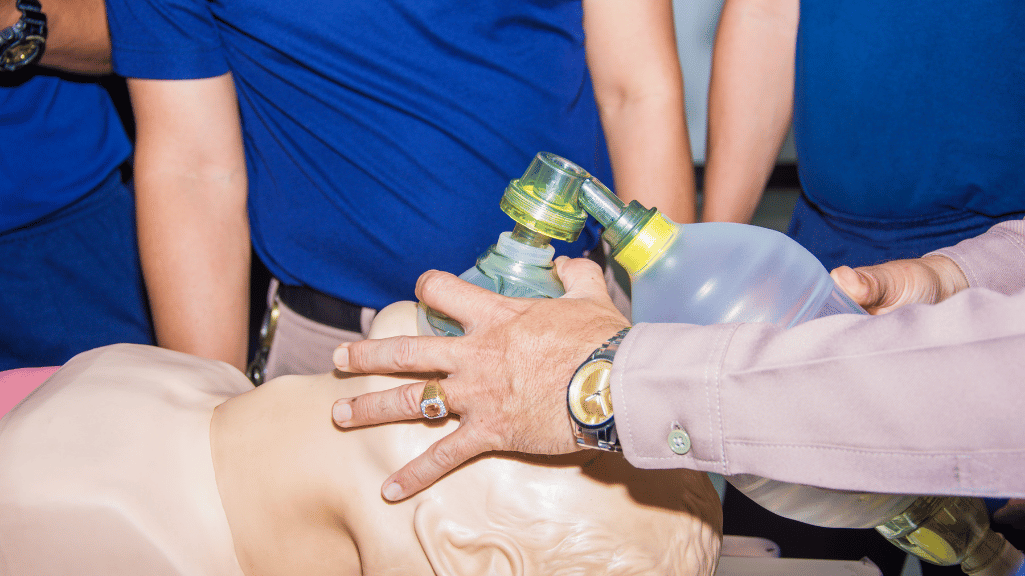
Breaths are delivered using a bag mask device by manually squeezing an oxygen-filled reservoir bag that is attached to an oxygen source and mask. The mask is firmly placed over the patient’s nose and mouth to form an airtight seal. With each squeeze of the bag, oxygen is forced from the reservoir bag through the one-way valve and into the patient’s lungs, providing ventilation. The opposite end of the bag is connected to 100% oxygen, which fills the bag for the next delivered breath. By rhythmically squeezing the bag, medical personnel can manually control the rate and volume of each breath delivered to the patient until other ventilation support can be provided.
What is a Bag-Mask?
The Bag-Valve Mask (BVM) device manually compresses the bag, forcing air or oxygen through the one-way valve into the patient’s lungs. The bag mask contains the following components:
- Self-Expanding Bag: The user squeezes the self-expanding bag, pushing air or oxygen through the valve. This self-inflating bag automatically refills with air or oxygen after compression.
- One-Way Valve: The one-way valve ensures that the air flows only toward the patient.
- Face Mask: The face mask is carefully positioned over the patient’s nose and mouth to create a mask seal.
- Release: Upon releasing the bag, it refills with air or oxygen, ready to be compressed again.
The process can be repeated to provide regular breaths to the patient until spontaneous breathing resumes or more advanced interventions are available.
When Are The Bag-Mask Needed?
Bag-mask ventilation is a critical component of resuscitation efforts in various medical emergencies. Some situations where bag-mask ventilation may be needed include:
- Cardiac Arrest:
In instances of cardiac arrest, while delivering basic life support (BLS) a bag-mask device can be used to provide controlled ventilation in tandem with chest compressions, ensuring oxygenation and carbon dioxide removal. - Pre-Hospital Emergency Care:
Emergency medical technicians and paramedics may use bag-mask devices to stabilize patients in respiratory distress while transporting them to the hospital.
- During Anesthesia:
Anesthesiologists use bag-mask ventilation as a temporary measure during induction and emergence from anesthesia, particularly if intubation is delayed or problematic. - Neonatal Resuscitation:
In neonatal intensive care units, bag-mask devices are often the first line of support for newborns who are not breathing adequately at birth. - Respiratory Failure in Chronic Illness:
Patients with chronic respiratory diseases like COPD or asthma who experience acute exacerbations may benefit from bag-mask ventilation until further treatment can be administered. - Drowning and Near-Drowning Incidents:
In drowning or near-drowning cases, a bag-mask device can provide ventilation. Using a proper ventilation technique ensures effective oxygen delivery during resuscitation. - Drug Overdose:
In cases of drug overdose where respiratory depression has occurred, bag-mask devices may be utilized to support breathing until the effects of the drugs have worn off or antidotes are administered. - Mass Casualty Incidents:
In scenarios involving mass casualties, where resources may be limited, bag-mask devices can be deployed for quick and efficient respiratory support for multiple patients. - High Altitude and Remote Areas:
In remote or high-altitude areas where advanced medical care might not be readily available, bag-mask devices can provide crucial support to individuals experiencing respiratory distress. - Training and Education:
Medical professionals, first responders, and even laypersons in some areas are trained in the use of bag-mask devices. They are a standard part of CPR and emergency response training. - Support During Advanced Procedures:
Sometimes bag-mask ventilation is used as a temporary support measure during procedures like bronchoscopy or certain diagnostic imaging, where anaesthesia is administered.
Instructions to Deliver Breath Using Bag-Mask
Before using a bag-mask, ensure the breathing aid is intact, understand its components, and assess the patient’s suitability. Secure consent if conscious, clear the airway, position the patient, coordinate with team members, and monitor responsiveness for effective ventilation. If a bag-mask is unavailable, mouth-to-mouth breathing can be used as an alternative to deliver oxygen. There are a lot of other instructions that make sure the effectiveness while delivering breath using the bag-mask device. We have explained all of the instructions in the correct order of steps for using a bag-mask device:
#1 Prepare Equipment and Patient
Check the Equipment: Ensure all parts of the resuscitation equipment, including the bag-mask device, are in good condition. This includes the self-expanding bag, one-way valve, face mask, and any additional components such as oxygen tubing or reservoir.
Connect to Oxygen (if available): If supplemental oxygen is required, connect the tubing to an oxygen source and adjust the flow rate as needed.
Position the Patient: Lay the patient on their back on a firm surface, ideally with the head slightly elevated.
#2 Position the Mask
Select the Appropriate Mask Size: Choose a mask that fits the patient’s face without covering the eyes or extending below the chin.
Hold the Mask: Use the “EC clamp” technique, with the thumb and index finger forming a “C” around the top of the mask and the other three fingers forming an “E” around the jaw.
Create a Seal: Place the mask over the patient’s nose and mouth, pressing down firmly to create a complete seal. Make adjustments as necessary to eliminate any leaks.
Must Read: When Using a Pocket Mask Where Should the Rescuer Be Positioned?
#3 Deliver the Breaths
Squeeze the Bag: Compress the bag smoothly and firmly, observing for chest rise to ensure air enters the lungs.
Control the Rate and Volume: Aim for an adult rate of 12 to 20 breaths per minute, with each breath delivered over approximately one second. Adjust volume to achieve visible chest rise without over-inflation.
Coordinate with Chest Compressions (if applicable): If CPR is in progress, ensure ventilation aligns with chest compressions. In scenarios requiring continuous chest compressions, provide breaths without interrupting compressions using advanced techniques.
Related Post: What is the Correct Volume of Air to Deliver During BVM Ventilations?
#4 Monitor the Patient
Watch for Chest Rise: Regularly assess the patient’s chest rise, color, and other vital signs to evaluate the effectiveness of ventilation.
Listen for Air Escape: If you hear air escaping, adjust the mask seal or the force of your compressions as needed.
Consider Advanced Airway if Needed: If bag-mask ventilation is inadequate, prepare for the possibility of advanced airway management like intubation.
#5 Maintain Safety and Hygiene
Protect from Aspiration: If the patient shows signs of vomiting or regurgitation, turn the head to the side to prevent aspiration and clean the airway as needed.
Avoid Over-Inflation: Over-inflating the lungs can cause barotrauma and should be avoided.
Clean and Disinfect: Follow appropriate protocols for cleaning and disinfecting the device after use.
#6 Transition to Advanced Care
Continue Monitoring: Keep a close eye on the patient’s response and be ready to adapt as the situation changes.
Coordinate with Other Medical Professionals: If more advanced care is needed, coordinate with other healthcare providers for a smooth transition to the next level of care.
Pros of Using Bag Mask
- Accessibility: Bag-mask devices are widely available and can be found in most medical settings, including ambulances and first-aid kits, ensuring quick access in emergencies.
- Cost-Effective: Compared to other respiratory support devices, bag-mask devices are relatively inexpensive, making them a practical option for many healthcare providers.
- Compatibility with Oxygen: The device can be connected to an oxygen source, allowing for the delivery of high concentrations of oxygen when needed.
- Use in Various Patient Groups: Suitable for adults, children, and infants with appropriate size adjustments.
- Adaptability: Can be used as a temporary measure while preparing for more advanced airway management techniques, such as intubation.
- Non-Invasive: As it doesn’t require insertion into the airway, it’s less invasive than some other breathing support options.
Cons of Using Bag-Mask
- Risk of Aspiration: If a patient vomits, there’s a risk of aspiration, as the device does not protect the airway.
- Ineffective Seal: It may be challenging to create an effective seal with the mask, especially in patients with facial hair, deformities, or obesity.
- Tiring for the Rescuer: Manual compression of the bag can be physically exhausting over time, potentially leading to decreased effectiveness.
- Potential for Barotrauma: Overly forceful or rapid ventilation may cause trauma to the lungs.
- Lack of Feedback: Unlike mechanical ventilators, bag-mask devices do not provide precise feedback about the volume or pressure of air delivered, which can lead to under or over-ventilation.
- Potential for Infection Spread: There can be a risk of infection transmission between patients if the tool is not cleaned properly.
- Interference with CPR: If used during cardiopulmonary resuscitation (CPR), it may interrupt chest compressions, affecting overall resuscitation efficacy.
Also Read: What Does the Chest Compression Feedback Device Monitor?
Conclusion
A bag-mask device is essential in emergency respiratory care, bridging the gap between the onset of a breathing problem and more advanced intervention. Its simple, life-saving design makes it essential in medical care. Online BLS classes and ACLS classes often emphasize the importance of understanding bag-mask ventilation. However, proper training and awareness of its limitations are crucial to maximizing its effectiveness. Contact us now: 877-846-8277
Frequently Asked Questions
How do you know that you are providing effective breaths when using a bag-mask device?
Effectiveness in providing breaths using a bag-mask device can be assessed through several indicators. Continuous observation and responsiveness to these indicators help ensure that breaths delivered through a bag-mask device effectively support the patient’s respiratory function. Regular reassessment is essential to make adjustments as needed and maintain adequate ventilation for optimal patient outcomes.
- Observe for visible chest rise with each ventilation. A rising chest indicates that the delivered breath is entering the lungs.
- Ensure a proper seal between the mask and the patient’s face. A secure seal helps prevent air leakage and ensures the delivered breath reaches the lungs.
- Listen for breath sounds using a stethoscope. Positive lung sounds confirm air entry into the lungs, indicating effective ventilation.
- Use capnography to monitor the end-tidal carbon dioxide (ETCO2) levels. Adequate ETCO2 indicates successful ventilation and suggests that carbon dioxide is being eliminated from the lungs.
- Monitor the patient’s overall response. An improvement in colour, heart rate, and oxygen saturation suggests effective ventilation.
- During exhalation, observe for chest fall. A visible fall indicates that the patient is exhaling and the lungs are emptied appropriately.
Assess the compliance of the bag. A bag that returns to its original shape after compression suggests proper ventilation mechanics.
What is the breath rate with a bag-mask device?
For a patient with a perfusing rhythm, provide 10-12 breaths per minute. While delivering cardiopulmonary resuscitation (CPR) give standard 2 breaths after 30 chest compressions. The recommended breath rate when using a bag-mask device depends on the age and condition of the patient. Here are the general guidelines for different demographic patients:
Adults: Provide 1 breath every 5 to 6 seconds, corresponding to approximately 10 to 12 breaths per minute.
Children: Deliver 1 breath every 3 to 5 seconds, resulting in a breath rate of 12 to 20 breaths per minute.
Infants: Administer 1 breath every 3 to 5 seconds, maintaining a breath rate of 12 to 20 breaths per minute.
What mask delivers 100% oxygen?
A non-rebreathing mask delivers nearly 100% oxygen by utilizing a reservoir bag and one-way valves. During inhalation, the valves facilitate the flow of oxygen from the reservoir bag to the patient’s lungs, preventing the inhalation of room air. Exhaled gases exit through vents, ensuring the patient does not rebreathe exhaled air.
This design minimizes the entrainment of room air, optimizing the delivery of high oxygen concentrations. Proper fit, valve integrity, and oxygen flow rate are critical for the device’s effectiveness in various medical scenarios, particularly in emergency and critical care settings.
Are bag-mask devices always successful?
A study from 2019 and 2020 gives us data on improved cardiac arrest episodes outside the hospital setting. When used correctly, the bag-mask device can make a difference. The research has also shown that the patients had higher oxygen saturation levels and lower rates of severely low oxygen levels.